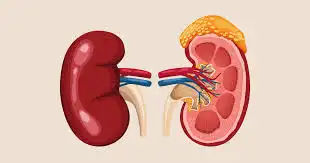
Overview
The kidneys are among the most vital organs in the human body. Working silently round the clock, they filter approximately 200 litres of blood every single day, removing toxins, balancing fluids, and maintaining the body’s internal chemistry. But what happens when the very filters inside the kidneys start to fail? This is precisely what occurs in a condition known as Glomerulonephritis — a group of diseases that cause inflammation in the kidney’s tiny filtering units called glomeruli.
Glomerulonephritis is not a single disease. It is an umbrella term that covers a range of conditions, all of which involve damage to the glomeruli. When these microscopic filtering units become inflamed or scarred, the kidneys can no longer do their job effectively. Proteins and red blood cells — which should stay inside the bloodstream — begin to leak into the urine. Waste products that should be filtered out start building up in the blood instead.
If left unaddressed, glomerulonephritis can progress to chronic kidney disease or even complete kidney failure. Yet many people living with this condition either do not know they have it or delay seeking proper care. This comprehensive guide is designed to help you understand everything about glomerulonephritis — from its root causes and warning signs, to accurate diagnosis and effective treatment options, including the role of homeopathy in managing this condition holistically.
What is Glomerulonephritis?
To understand glomerulonephritis, it helps to first understand how the kidneys work. Each kidney contains roughly one million tiny filtering units called nephrons. Each nephron includes a glomerulus — a small cluster of capillaries (tiny blood vessels) surrounded by a cup-shaped structure called Bowman’s capsule. Blood flows through the glomerulus under pressure, and the walls of the capillaries act as a sieve, allowing small molecules like water, salts, and waste products to pass through while holding back larger molecules like proteins and blood cells.
In glomerulonephritis, this delicate filtering membrane becomes inflamed. The inflammation may be triggered by the immune system attacking the kidneys, infections, certain medications, or underlying systemic diseases. Once inflamed, the glomerular membrane becomes leaky or damaged, allowing substances that should remain in the blood to spill into the urine. At the same time, harmful waste products that should exit the body through urine begin accumulating in the bloodstream, leading to a cascade of health problems throughout the body.
The word ‘glomerulonephritis’ itself comes from Latin and Greek roots: ‘glomerulus’ (a small ball or cluster), ‘nephros’ (kidney), and ‘itis’ (inflammation). The condition is also sometimes referred to as glomerular disease or nephritis.
Types of Glomerulonephritis
Glomerulonephritis is broadly classified into two major categories based on its onset and duration:
1. Acute Glomerulonephritis
Acute glomerulonephritis develops suddenly, often following an infection such as streptococcal throat infection (strep throat) or skin infection. This form is more commonly seen in children, though adults can also be affected. In many cases of acute post-infectious glomerulonephritis, the kidney inflammation resolves once the underlying infection is treated. However, without timely care, even acute cases can cause lasting kidney damage.
2. Chronic Glomerulonephritis
Chronic glomerulonephritis develops gradually over months or years, often without causing obvious symptoms in the early stages. It may follow an episode of acute glomerulonephritis that did not resolve completely, or it may develop insidiously due to genetic factors, autoimmune conditions, or other diseases. Over time, chronic glomerulonephritis leads to progressive scarring of the glomeruli, steadily reducing the kidney’s filtering capacity. This is one of the leading causes of end-stage renal disease (kidney failure) worldwide.
Beyond this broad classification, glomerulonephritis is also categorised based on the specific pattern of damage seen under a microscope, including:
- IgA Nephropathy (Berger’s Disease) — the most common form globally, caused by deposits of IgA antibodies in the glomeruli.
- Minimal Change Disease — primarily affects children; the glomeruli appear normal under a regular microscope but show abnormalities under electron microscopy.
- Focal Segmental Glomerulosclerosis (FSGS) — scarring affects only some glomeruli and only parts of each affected glomerulus.
- Membranous Nephropathy — thickening of the glomerular membrane due to immune complex deposits.
- Rapidly Progressive Glomerulonephritis (RPGN) — a severe, fast-worsening form that can cause kidney failure within weeks if not treated urgently.
- Lupus Nephritis — glomerular inflammation caused by systemic lupus erythematosus (SLE).
What Causes Glomerulonephritis?
Glomerulonephritis can arise from a wide variety of causes. In many cases, it develops because the immune system mistakenly targets the kidneys — either directly or as a result of immune complexes (clumps of antibodies and antigens) becoming trapped in the glomeruli and triggering inflammation. The major causes include:
Infections
Bacterial infections, particularly those caused by Group A Streptococcus (the same bacteria responsible for strep throat and impetigo), are a well-known trigger for acute post-streptococcal glomerulonephritis. Viral infections such as hepatitis B, hepatitis C, and HIV can also cause chronic forms of glomerulonephritis by triggering abnormal immune responses that damage the kidneys over time.
Autoimmune Diseases
In autoimmune conditions, the body’s immune system turns against its own tissues. Systemic Lupus Erythematosus (SLE), a chronic autoimmune disease, frequently involves the kidneys, causing lupus nephritis. Similarly, conditions like Goodpasture syndrome, where the immune system attacks the glomerular basement membrane, can cause rapidly progressive and potentially life-threatening glomerulonephritis.
Vasculitis
Vasculitis refers to inflammation of the blood vessels. Certain vasculitic conditions such as ANCA-associated vasculitis (granulomatosis with polyangiitis, microscopic polyangiitis) directly attack the small blood vessels in the glomeruli, causing severe and rapidly worsening kidney damage.
Other Contributing Factors
- Diabetes mellitus — chronic high blood sugar damages glomerular capillaries over time (diabetic nephropathy).
- High blood pressure — uncontrolled hypertension strains the glomerular capillaries and accelerates damage.
- Genetic conditions — inherited disorders such as Alport syndrome weaken the structural proteins of the glomerular membrane.
- Certain medications — long-term use of NSAIDs (non-steroidal anti-inflammatory drugs) and some antibiotics can harm the kidneys.
- Idiopathic causes — in a significant number of cases, no clear cause can be identified despite thorough investigation.
Signs and Symptoms of Glomerulonephritis
One of the challenges of glomerulonephritis is that its symptoms can be subtle, especially in the early or chronic stages. Many people do not realise anything is wrong until the condition has already caused significant kidney damage. The symptoms vary depending on whether the disease is acute or chronic and how severely the glomeruli are affected.
Urinary Changes
Blood in the urine (haematuria) is one of the most telling signs of glomerulonephritis. The urine may appear dark brown, tea-coloured, or smoky — a classic description associated with post-streptococcal glomerulonephritis. Protein leaking into the urine (proteinuria) can cause the urine to appear foamy or frothy. Reduced urine output (oliguria) may also occur when kidney function is significantly impaired.
Swelling (Oedema)
When the kidneys fail to filter properly, sodium and water accumulate in the body, leading to fluid retention. This typically manifests as puffiness around the eyes (especially noticeable in the morning), swelling of the face, hands, feet, and ankles, and in severe cases, fluid accumulation in the abdomen or lungs.
High Blood Pressure
Glomerulonephritis often causes hypertension because damaged kidneys struggle to regulate blood pressure and fluid balance. Elevated blood pressure, in turn, accelerates glomerular damage, creating a dangerous cycle that further worsens kidney function.
Fatigue and General Weakness
As kidney function declines and waste products accumulate in the blood, individuals often experience persistent fatigue, weakness, reduced concentration, and a general sense of feeling unwell. Anaemia (low haemoglobin levels) may also develop because damaged kidneys produce less erythropoietin, the hormone that stimulates red blood cell production.
Other Symptoms
- Nausea and vomiting in advanced kidney disease
- Loss of appetite and unintentional weight loss
- Headaches associated with elevated blood pressure
- Shortness of breath if fluid accumulates around the lungs
- Joint or muscle aches, particularly in cases associated with lupus or vasculitis
How is Glomerulonephritis Diagnosed?
Accurate diagnosis is the cornerstone of effective management. Glomerulonephritis requires a combination of clinical evaluation, laboratory investigations, and in many cases, a kidney biopsy. The diagnostic process typically involves the following steps:
Urine Analysis (Urinalysis)
A routine urine test is usually the first step. The presence of red blood cells, red cell casts (cylindrical structures formed when blood cells stick together in the kidney tubules), and protein in the urine strongly suggests glomerulonephritis. A 24-hour urine protein test may be performed to quantify the amount of protein being lost.
Blood Tests
Blood tests help assess how well the kidneys are functioning and identify potential causes. Key tests include serum creatinine and blood urea nitrogen (BUN) levels, which rise when kidney filtration is impaired. Glomerular filtration rate (GFR) calculation helps stage the level of kidney function. Tests for antinuclear antibodies (ANA), anti-double-stranded DNA antibodies, ANCA, and complement levels help identify autoimmune causes.
Imaging Studies
Ultrasound of the kidneys helps evaluate their size, shape, and structure. Kidneys that have become scarred and shrunken indicate chronic disease, while normal or enlarged kidneys suggest acute disease. In some cases, CT scans or MRI may be used to get more detailed imaging.
Kidney Biopsy
A kidney biopsy is the most definitive diagnostic tool for glomerulonephritis. A small sample of kidney tissue is obtained using a fine needle under ultrasound guidance and examined under light microscopy, electron microscopy, and immunofluorescence microscopy. This reveals the precise type and pattern of glomerular damage, which is essential for guiding treatment decisions.
Conventional Treatment Approaches
Conventional medicine focuses on controlling symptoms, slowing the progression of kidney damage, and treating any underlying cause. Treatment options depend on the type and severity of glomerulonephritis:
- Immunosuppressive therapy — corticosteroids (such as prednisolone) and other immunosuppressive agents like cyclophosphamide or mycophenolate mofetil are used to reduce immune-mediated kidney inflammation in conditions such as lupus nephritis, FSGS, and RPGN.
- Antihypertensive medications — ACE inhibitors (such as enalapril) and ARBs (such as losartan) are particularly beneficial as they not only lower blood pressure but also reduce proteinuria and have a kidney-protective effect.
- Diuretics — to manage fluid retention and oedema by promoting the excretion of excess sodium and water through urine.
- Dietary modifications — a low-sodium, low-protein diet helps reduce the workload on damaged kidneys and controls fluid retention.
- Treatment of underlying infections — antibiotic therapy for streptococcal infections, antiviral therapy for hepatitis B or C.
- Dialysis or kidney transplantation — in end-stage renal disease where the kidneys can no longer sustain life.
While these treatments are important and sometimes lifesaving, they also carry significant side effects, particularly with long-term use of corticosteroids and immunosuppressants. This is one reason why many patients explore complementary approaches such as homeopathy alongside conventional care.
Homeopathic Treatment for Glomerulonephritis in Lucknow, India
Homeopathy is a system of medicine based on the principle that ‘like cures like’ — substances that can produce symptoms in a healthy person can, in highly diluted form, stimulate the body’s own healing mechanisms to address similar symptoms in a sick person. Homeopathy treats the whole person rather than the disease in isolation, taking into account the individual’s physical complaints, emotional state, general constitution, and personal and family medical history.
In glomerulonephritis, homeopathic treatment aims to reduce inflammation in the kidneys, minimise protein and blood loss in the urine, support overall kidney function, manage associated symptoms such as oedema and high blood pressure, and improve the patient’s general vitality and immunity. It is important to note that homeopathy works best as a complementary approach — supporting and enhancing the body’s healing capacity — and should always be used under the guidance of a qualified homeopathic practitioner, alongside necessary conventional monitoring and care.
Commonly Used Homeopathic Medicines for Glomerulonephritis
The following medicines are among those that an experienced homeopathic physician may consider when managing glomerulonephritis. The selection of medicine is always highly individualised and should never be self-prescribed without proper consultation.
Apis Mellifica
Derived from the honey bee, Apis Mellifica is a key remedy for conditions involving significant fluid retention and oedema. It is indicated when there is marked swelling around the eyes, face, and extremities, with scanty, dark, and sometimes bloody urine. The patient may feel a burning or stinging sensation in the kidneys. It is particularly useful in early or acute stages of glomerulonephritis where oedema is a prominent feature.
Arsenicum Album
Arsenicum Album is one of the most widely used homeopathic remedies for kidney diseases involving significant protein loss and general debility. It is indicated in patients who experience profound weakness and exhaustion, burning sensations in the kidneys, frothy urine with large amounts of albumin, and significant puffiness of the face and extremities. The patient is typically anxious, restless, and feels worse at night.
Berberis Vulgaris
Berberis Vulgaris, derived from the barberry plant, has a strong affinity for the kidneys and urinary tract. It is commonly indicated when there is aching or radiating pain in the kidney region, changes in urine colour, and urinary symptoms that worsen with pressure on the kidney area. It helps support kidney function and promotes healthy elimination.
Phosphorus
Phosphorus is considered an important constitutional remedy for glomerulonephritis, particularly when there is significant proteinuria (albuminuria), haematuria, and progressive kidney weakness. It is suited to individuals who are sensitive, sympathetic, and tend to become easily tired. The urine may be dark, turbid, or contain fatty droplets. Phosphorus helps address the degenerative tendency in the kidneys and supports tissue repair.
Terebinthina
Terebinthina is specifically indicated when blood in the urine (haematuria) is a prominent symptom. The urine may appear smoky, dark, or resemble the colour of coffee grounds — a hallmark description of glomerulonephritis-related haematuria. There may be a burning sensation and inflammation along the entire urinary tract. It is one of the most frequently indicated remedies in the acute stages of glomerulonephritis presenting with visible blood in urine.
Helonias Dioica
Helonias Dioica is a valuable remedy for kidney conditions accompanied by heavy proteinuria, profound weakness, and a characteristic sense of weight and dragging in the kidney region. It is often indicated in patients whose kidney function is declining with progressive albuminuria, and who experience extreme fatigue that is temporarily improved by mental distraction or activity.
Mercurius Corrosivus
Mercurius Corrosivus is a powerful remedy for conditions with severe haematuria, intense burning, and significant urinary involvement. It is indicated when the urine contains blood and albumin in large quantities, and there is a burning sensation in the kidneys that extends through the urinary passage. This remedy is especially useful in severe or rapidly progressing cases of glomerulonephritis.
Why Choose Homeopathy for Glomerulonephritis?
Many patients and families seek homeopathic care for glomerulonephritis for several compelling reasons. Firstly, homeopathic medicines are gentle, non-toxic, and free from the significant side effects associated with long-term steroid and immunosuppressant use. Secondly, homeopathy does not merely suppress symptoms — it addresses the underlying constitutional susceptibility that makes an individual prone to kidney disease, thereby offering a more root-level correction.
Homeopathy also considers the whole person — physical, mental, and emotional — rather than focusing exclusively on the kidneys in isolation. This holistic approach often results in improvements in the patient’s overall sense of wellbeing, energy levels, emotional resilience, and quality of life, even as it works to support kidney health. For patients who are unable to tolerate conventional medications or are looking for a safe adjunct to their existing treatment, homeopathy offers a meaningful option.
Diet and Lifestyle Guidance for Glomerulonephritis
Diet plays a crucial role in managing glomerulonephritis and protecting kidney function. The following evidence-based dietary and lifestyle recommendations can help slow the progression of the disease and improve quality of life:
- Limit sodium intake — reducing salt in the diet helps control fluid retention, swelling, and blood pressure. Avoid processed foods, pickles, papads, and packaged snacks, which are typically high in sodium.
- Moderate protein intake — in kidney disease, the kidneys struggle to process the waste products of protein metabolism. Moderate reduction in dietary protein (under medical guidance) can help reduce the burden on the kidneys.
- Control potassium and phosphorus — as kidney function declines, the body may struggle to excrete excess potassium and phosphorus. Foods such as bananas, oranges, potatoes, dairy products, and nuts may need to be consumed in moderation.
- Stay adequately hydrated — drink sufficient water to support urinary function, but avoid excessive fluid intake if urine output is reduced or oedema is present.
- Maintain a healthy weight — obesity places additional strain on the kidneys and worsens hypertension and proteinuria.
- Control blood sugar — in patients with diabetes, strict blood glucose control is essential to prevent further glomerular damage.
- Avoid smoking and alcohol — both are harmful to kidney function and overall cardiovascular health.
- Exercise moderately — gentle, regular physical activity supports cardiovascular health and blood pressure control, but should be tailored to individual capacity.
- Regular kidney function monitoring — periodic blood and urine tests are essential to track disease progression and assess the response to treatment.
Complications of Untreated or Poorly Managed Glomerulonephritis
If glomerulonephritis is not diagnosed early and managed effectively, it can lead to a range of serious complications. Chronic kidney disease (CKD) is the most common long-term consequence, characterised by a gradual, irreversible decline in kidney function. End-stage renal disease (ESRD) represents the most severe stage, where the kidneys can no longer sustain life and the patient requires permanent dialysis or kidney transplantation.
Other complications include nephrotic syndrome (characterised by massive protein loss, severe oedema, high cholesterol, and increased susceptibility to infections), hypertensive emergencies due to dangerously elevated blood pressure, increased risk of cardiovascular disease, and in children, developmental delays or growth retardation in severe cases.
FAQs about Glomerulonephritis
Is glomerulonephritis curable?
Some forms of glomerulonephritis — particularly acute post-streptococcal glomerulonephritis in children — can resolve completely with appropriate treatment. However, many forms of chronic glomerulonephritis are not fully curable but can be effectively managed to slow progression, preserve kidney function, and maintain a good quality of life. Early diagnosis and consistent management are key.
Can children get glomerulonephritis?
Yes, glomerulonephritis can affect people of all ages, including young children. Post-streptococcal glomerulonephritis and minimal change disease are particularly common in childhood. Children often have a better prognosis than adults, especially when diagnosed and treated early.
Is glomerulonephritis painful?
Glomerulonephritis does not typically cause acute sharp pain, but some patients may experience a dull aching sensation in the kidney region (the flank or lower back). The main discomfort usually comes from symptoms such as swelling, fatigue, and high blood pressure rather than direct kidney pain.
Can homeopathy be used alongside conventional treatment for glomerulonephritis?
Yes, homeopathy can be used as a complementary approach alongside conventional kidney disease management. It does not interfere with prescribed medications and can help support kidney health, manage symptoms, reduce the side effects of conventional drugs, and improve overall wellbeing. However, it is essential that both your nephrologist and homeopathic physician are aware of all treatments you are receiving.
How often should someone with glomerulonephritis have check-ups?
The frequency of monitoring depends on the type and severity of glomerulonephritis. In acute cases, check-ups may be needed every few weeks initially. In stable chronic cases, quarterly blood and urine tests are typical. Your physician will advise on the appropriate monitoring schedule based on your individual condition.
Conclusion
Glomerulonephritis is a serious but manageable condition when approached with awareness, timely diagnosis, and comprehensive care. Whether you or a loved one has been recently diagnosed, are seeking a second opinion, or are looking for complementary support alongside conventional treatment, understanding the nature of this disease is the critical first step.
Homeopathy offers a safe, personalised, and holistic approach that addresses not just the kidney inflammation but the whole individual — their constitution, their immune response, their emotional health, and their overall vitality. Combined with appropriate dietary changes, lifestyle modifications, and necessary conventional monitoring, homeopathic treatment can play a meaningful role in supporting kidney health and improving quality of life in glomerulonephritis.
If you are in Lucknow or surrounding areas and seeking expert homeopathic consultation for glomerulonephritis or other kidney conditions, please reach out to our clinic for a detailed, personalised evaluation. Our experienced team of doctors is committed to providing compassionate, evidence-informed homeopathic care that works alongside modern medicine to give you the best possible outcomes.
Why choose Dr. Sanjay’s Homoeopathy for Glomerulonephritis Treatment in Lucknow, India?
Dr. Sanjay’s Homoeopathy is a trusted clinic for safe and effective Glomerulonephritis treatment in Lucknow, India. With more than 22 years of experience, Dr. Sanjay Singh, MD (Homoeopathy), provides specialized homeopathy treatment that helps manage blood in urine, swelling, high blood pressure, reduced kidney function, fatigue, and protein leakage naturally without side effects. As a leading homeopathic doctor in Lucknow, he follows international treatment standards and offers a personalized approach that focuses on reducing kidney inflammation, supporting filtration function, slowing disease progression, and preventing complications, making him the best homeopathy doctor for Glomerulonephritis in Lucknow. Patients from across India and around the world choose Dr. Sanjay’s Homoeopathy for its holistic healing, long-lasting relief, and compassionate care in managing kidney conditions like Glomerulonephritis.


